Passive congestion (Passive hyperemia) (lung)
Hyperemia (congestion) represents the increase of blood in a territory, due to dilatation of small vessels. According to the mechanism, it may be active or passive.
Active hyperemia (congestion) is a result of arteriolar distension (e.g., skeletal muscle activity, inflammation, local neuro-vegetative reaction).
Passive hyperemia (congestion), also termed stasis, is a consequence of an impaired venous drainage (heart failure, compression or obstruction of veins), followed by dilatation of venules and capillaries.
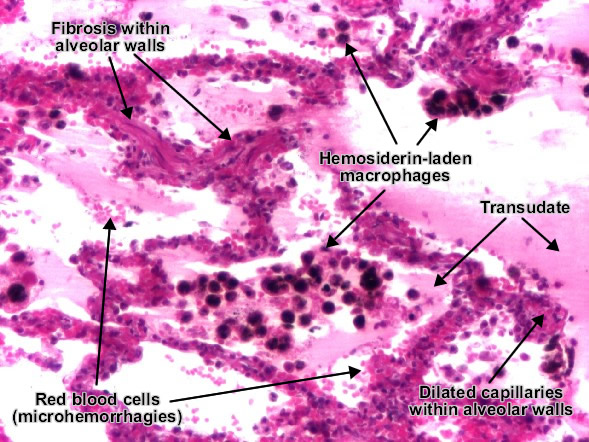
Etiology of passive congestion of the lung : chronic left heart (ventricular) failure.
Alveolar walls are thickened due to dilated capillaries. Alveolar lumens are filled with transudate (amorphous, eosinophilic and homogenous) which replaced the air, red blood cells (microhemorrhages) and hemosiderin-laden macrophages (also called "heart failure cells"). (H&E, ob. x20)
With progression, interstitial fibrosis may appear and, together with hemosiderin pigmentation, generates the aspect of "brown induration". Extensive fibrosis leads to intrapulmonary hypertension.
Passive congestion (Passive hyperemia) (lung) (detail)
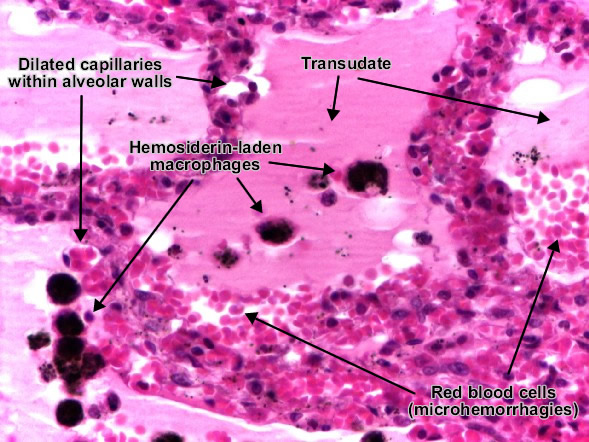
Passive congestion of the lung. Hemosiderin-laden macrophages contain in cytoplasm hemosiderin pigment (brown, granular), resulted from destruction of red blood cells in alveolar lumen. (H&E, ob. x40)
Perls reaction is useful in distinguishing hemosiderin pigment from anthracotic (carbon) pigment : trivalent iron from hemosiderin stains in green-blue, while anthracotic pigment remains dark-brown and is mainly located perivascular.
Additional information :